Arsenic Contamination of Groundwater in Nepal: Good Public Health Intention Gone Bad
By
2012, Vol. 4 No. 09 | pg. 1/3 | »
IN THIS ARTICLE
KEYWORDS
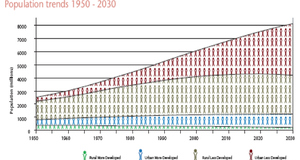
Nepal is a small developing country in South Asia, bordered by China to the north and India to the south, east and west. With a total land area of 56,827 square miles, the country is predominantly mountainous with more than 80% of the total area covered by hills and mountains. However, the southern belt of Nepal consists of flat alluvial plains called the Terai region, populated by almost half of the total population of the country.1 According to the Central Intelligence Agency (CIA) census, 2012, the estimated total population of the country is 29,890,686 with growth rate of 1.768% per annum.2 More than half of the Nepalese population lives below the international poverty line.3 Of the many health issues that plague the country, none is more important than the prevalence of waterborne illness. One of the main reasons for its widespread occurrence is that more than 70% of the population does not have access to clean, safe drinking water.4 About 47% of Nepal’s total population lives in Terai region and 90% of them rely on groundwater as their major source of drinking water. In the mid 1980s, more than 200,000 shallow tube wells were installed by different governmental and non-governmental agencies to serve drinking water to 11 million people residing in the region.5 Until the mid-1990s, most of the tube wells were reported to be bacteriologically safe for drinking water purposes, primarily, because the test was limited to iron, ammonia, nitrate and coliform test. The issue of arsenic contamination in drinking water of Terai region in Nepal became a major focal point after the emergence of arsenic contamination in groundwater of the Bengal Delta Plain (BDP) in the neighboring Indian State of West Bengal and Bangladesh.6 Although contamination of tube well water by arsenic in this area was first reported in 1999, not much attention has been given to this subject. Arsenic contamination of natural waters has become an issue of growing concern, particularly in Southeast Asia, to the extent that the World Health Organization (WHO) declared groundwater contamination on the Bengal delta the largest mass poisoning of a population in history.7 Because much of southern Nepal lies within the same Ganges drainage basin as West Bengal and western Bangladesh, Nepal is also one of the epicenters of the problem.1 The problem in Nepal is limited to the Terai region, that covers about 20 districts where 29% of tube wells have arsenic concentrations exceeding the WHO standard (10 g/L) with approximately 0.5 million people at risk of consuming water with an arsenic concentration > 50 mg/L.8 Studies have shown that the number of arsenic contaminated wells is rising, signifying arsenic poisoning as one of the major public health threats in Nepal.Health IssuesArsenic (As) is a ubiquitous element, which occurs naturally in the earth’s crust. Its source is geological in nature, as well as human activities such as mining, burning of fossil fuels, and pesticide application.9 In Nepal, the alluvial sediments deposited by rivers draining from the Himalayas have been implicated as the major source of arsenic in groundwater lying in the flat plain of Terai.10 Both inorganic and organic forms of arsenic have been identified in water by many researches around the world. Since ancient times, Arsenic has long been known as toxic, and its effects on health even at small doses can be quite harmful. Inorganic arsenics are proven as carcinogens in humans.8 The crises in India and Bangladesh provides frightening testament to the far-reaching, chronic effects of arsenic poisoning. Arsenic can be exposed to the human body through inhalation, ingestion and dermal absorption. 11 Inhalation takes place through respiration whereas ingestion occurs by the digestion of contaminated water and food, the primary course of exposure. Dermal absorption takes place due to the direct contact of arsenic compounds with the skin. Whatever the sources and the modes of exposure are, the total impact depends upon the duration of absorption, excretion and retention in the body as well as the concentration and the chemical nature of the element.12 The toxicity of arsenic to human health ranges from skin lesions to cancer of the brain, liver, kidney, and stomach. Arsenic can also be passed from a pregnant woman to her unborn child.3 The symptoms of the adverse health consequences of arsenic poisoning can be divided up into the acute and the chronic effects.13 Signs of acute poisoning manifest immediately if the dose is large enough and can occur within 30 minutes of entry into the body. Initial symptoms can include muscle pain, and weakness, followed by severe nausea, abdominal pain and diarrhea. Other symptoms include numbness in hands and feet, red rashes on the skin, intense thirst, decreased urine output, drowsiness and confusion, paranoid delusions, hallucinations, and delirium. However, doses from 60 to 180 mg can lead to seizures, coma and death. It can also cause gastrointestinal and cardiac damage and can affect the respiratory tract, the skin of the body, and cause numerous other severe health problems.14 In the initial stage of chronic exposure of arsenic for more than five years, skin color becomes black (melanosis), rough and tough (keratosis), eyes become red (conjunctivitis), bronchitis and gastroenteritis can occur in some cases.6 The manifestations of arsenicosis are clearer in the second stage with black and white spots on the skin (leukomelanosite), hard nodules on palms and soles (hyperkeratosis), swelling of legs, peripheral neuropathy and complications of kidney and liver.15 Hyperkeratosis appears predominantly on the palms and plantar aspect of feet. In addition to skin manifestation, arsenic poisoning also causes cancer of the bladder, kidneys, and lungs. Sometimes, it even causes neurological deficits and diabetes mellitus. People also complain of weakness, headache, burning of eyes and pain abdomen.16 Prevalence in NepalIn Nepal, there is a serious problem with arsenic contamination particularly in Terai region, worst being in Nawalparasi and its neighboring districts (Rautahat, Kailali, and Siraha), where 26% of shallow wells failed to meet the WHO’s standard of 10 ppb.17 An alarming 14.9% of tube wells had arsenic greater than 50µg/L. One well had arsenic concentrations of 2,620µg/L - the highest reading in the region - 262 times the WHO standard value.18 It is estimated that about 2.6 % of the total population, exposed to arsenic contaminated water with a concentration more than 50 ppb, have a prevalence of arsenicosis.6 In the regions, namely Nawalparasi, Bara, Parsa, Rautahat, Rupandehi, and Kapilvastu, the prevalence of arsenicosis is, on average, 2.2%. In the community-based study, the highest prevalence (18.6%) of arsenicosis was found in Patkhouli village of Nawalparasi, where 95.8% of tube wells were contaminated with arsenic.19 The prevalence of arsenicosis related dermatosis (skin disease) was 1.3 to 5.1% of the population and was higher in older age groups (>50 years) of both the sexes.5 All patients showed symptoms of melanosis (early stages of arsenic poisoning) and keratosis (mild stages of arsenic poisoning) on the palms, trunk, and soles of the feet.20 Males suffered more from arsenicosis than females (odds ratio: 2.50). Skin manifestations, such as melanosis and keratosis, were the common symptoms of arsenicosis.19 Most patients were identified in the early or mild stage of the disease. Clinical observation revealed melanosis with other manifestation in 95.6% and keratosis in 57.8% of the patients. Leucomelanosis (black and white spotsonthe legs andtrunk) was identified in 3.3% of the population.20 It was estimated that approximately 12.5 disability adjusted life years (DALYs) per 1000 population in Nepal is due to excess arsenic in the drinking water (arsenic concentration >50 μg/L).21 Arsenic poisoning can be diagnosed through samples of blood, urine, hair, and fingernails. The urine test is the most reliable test that needs to be done within 24–48hours for an accurate analysis of an acute exposure. Tests on hair and fingernails can measure exposure to high levels of arsenic over the past 6–12 months.22 These tests can determine if one has been exposed to above-average levels of arsenic. Chelation therapy is used to treat chronic arsenic poisoning that uses dimercaprol and dimercaptosuccinic acid as chelating agents.23 The beneficial effect of oral supplementation with Vitamin A (Retinol) has been described in the treatment of cutaneous arsenicosis. In addition, treatment in hospital with good nutritious diet like high proteins has been found to reduce symptom.24Continued on Next Page » Suggested Reading from Inquiries Journal
Inquiries Journal provides undergraduate and graduate students around the world a platform for the wide dissemination of academic work over a range of core disciplines. Representing the work of students from hundreds of institutions around the globe, Inquiries Journal's large database of academic articles is completely free. Learn more | Blog | Submit Latest in Health Science |