Featured Article:Mobile Phone Contamination by Microorganisms in Health Facilities: Comparing Health Care Workers and Patient Visitors in a Post-Operative Pediatric ICU
By
2012, Vol. 4 No. 08 | pg. 1/1
IN THIS ARTICLE
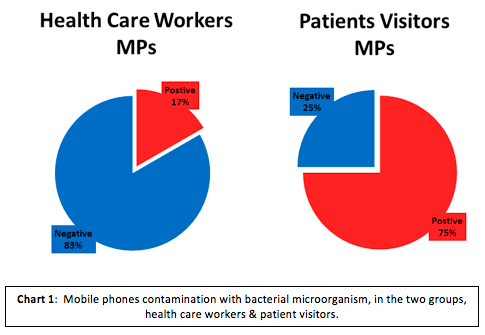
AbstractBackground: Mobile phones (MPs) come in close contact with the body and serve as a ready surface for colonization. The aim of this study was to compare MP colonization by bacterial microorganisms between Health Care Workers (HCWs) and Patients Visitors (PVs), in the Post-Operative Pediatric Intensive Care Unit (POPICU) of Children's Hospital, Ain Shams University in Cairo, Egypt. Mobile communications and wireless data transmission play an important role in health care facilities (Lapinsky & Easty, 2006). They come in close contact with the body and serve as a ready surface for colonization (Srikanth et al., 2010). Elkholy et al. (MT & IE, 2010) found a colonization rate reaching as high as 96.5% of MP colonization with bacteria in a previous study in Saudi Arabia. Ugler et al. demonstrated the use of MPs by HCWs in daily practice, as a source of nosocomial infections (NI) in hospitals. They also demonstrated the rate of routine cleaning of HCWs' MPs was 10.5% (Ulger et al., 2009). Nosocomial infection represents an important cause of morbidity and mortality for children admitted in the Pediatric Intensive Care Unit (PICU) (Brown, Stechenberg, Sands, Hosmer, & Ryczak, 1987), the overall mortality attributable to NI has been estimated at 11% (Milliken et al., 1988).The aim of this study was to measure MP colonization by bacterial microorganism, between HCWs and PVs, in POPICU at Children’s Hospital, Ain Shams University in Cairo, Egypt. MethodologyA cross section observational analytical study was carried out in POPICU during the period from 14th April 2011 to 21st April 2011 at the Children's hospital, Ain Shams University, Cairo, Egypt. Mobile phones of 18 HCWs and 8 PVs were included, swabs from 20 MPs were taken. All participants were not previously informed by the date of collecting the samples. Oral consents were taken from all the 20 participants who agreed for a swab to be taken from their MPs. All swabs have been taken only from the participants' MPs, whom were in the PSPICU at the time of screening. Three doctors and three nurses were excluded from screening as they were not carrying MPs or at holiday on screening time. A sterile swab moistened with sterile saline was rotated over the two surfaces and all sides of MPs. These samples were transferred for culture within 60 minutes from the first sample taken to a laboratory. All samples were cultured on MacConkey and Blood agars and incubated at 37◦C for 24 hours. Colonies from positive cultures were identified by film stained with Gram stain and biochemical reactions from Gram negative organisms. Those procedures were conducted by infection control unit in Children's Hospital, Ain Shams University, Cairo, Egypt. ResultsContamination of all MPs with microorganisms represented rate of 40% (=8). No microorganism growth was identified in 60% (=12) of MPs. The contamination of MPs of PVs group with microorganisms were 75% (=6), while the MPs of HCWs were ≈17% (=2) (chart 1). By Comparison, mobile phones of PVs show more contamination with microorganism than these of HCWs (p-value <0.02). While comparing the 2 groups with pathological micro-organisms, mobile phones of PVs show also more contamination than HCWs MPs. Gram positive bacteria were isolated from 15% of MPs, and Gram negative bacteria were isolated from 25% of MPs. Klebsiella spp., Anthracoid bacilli, Diphtheroid bacilli and Bacteroides spp. were representing 37.5%, 14.3%, 14.3% & 37.5% respectively of all contaminated MPs.
Discussion and ConclusionThere have always been restrictions on electronic device use in health care facilities because of the fear of electromagnetic interference with electronic medical devices; however, many health care facilities now allow the use of MPs. The possible transmissions of nosocomial pathogens by electronic devices were previously reported (Bellamy, Laban, Barrett, & Talbot, 1998; Isaacs, Daley, Dalton, Hardiman, & Nallusamy, 1998). Chin et al. reported MPs as an important way for patients and PVs to interface with outside world (Chin, Adams Jr, Khoury, & Zurakowski, 2005).In PSPICU, it is essential for the patient’s parents to be there and accompanying their children for some time. Several reports (Borer et al., 2005 ; Brady et al., 2006 ; Goldblatt et al., 2007 ; Karabay et al., 2007; Jayalakshmi et al., 2008; Sepehri et al., 2009; and Elkholy et al., 2010) have documented the contamination of MPs among HCWs (Borer et al., 2005; Brady, Wasson, Stirling, McAllister, & Damani, 2006; Goldblatt J. G. et al., 2007; Jayalakshmi, Appalaraju, & Usha, 2008; Karabay, Koçoglu, & Tahtaci, 2007; MT & IE, 2010; Sepehri, Talebizadeh, Mirzazadeh, Mir-shekari, & Sepehri, 2009). Tekerekoglu et al. (Tekerekoglu et al., 2011) suggested MPs belonging to patients & PVs are possible sources of microorganism contamination. Our study reported that there is significant higher contamination in MPs of PVs group (75%), compared to the MPs of HCWs were (16.7%); (p-value<0.02). According to Tekerekoglu et al. (Tekerekoglu et al., 2011), there were multidrug resistant pathogens on the patients’ MPs including MRSA and extended-spectrum beta-lactamase-producing E. coli and many others besides Klebsiella spp. However, Klebsiella spp. was the main organism found in our study (37.5%) besides the gram negative bacteroides spp. (37.5%) in the MPs of PVs. Our research presents higher contamination of MPs with pathological microorganism of PVs than HCWs. According to our results, it is essential to reduce bacterial colonization on the MPs. This can be made true by generalizing infection control guidelines to all HCWs and PVs. However, sensitivity to liquid and high temperature of many MPs limits their frequent disinfection. As our results suggest that MPs of PVs represent higher risk for bacterial colonization than those of HCWs, we suggest MPs of PVs should be left outside the PSPICU with adequate washing of PVs hands. Study limitations are important to be mentioned, that no molecular tests were conducted for determining clonal relation and no antibiotic sensitivity test were done. ReferencesBellamy, K., Laban, K., Barrett, K., & Talbot, D. (1998). Detection of viruses and body fluids which may contain viruses in the domestic environment. Epidemiology and infection, 121 (3), 673-680. Borer, A., Gilad, J., Smolyakov, R., Eskira, S., Peled, N., Porat, N., . . . Schlaeffer, F. (2005). «Cell phones and Acinetobacter transmission.». Emerg. Infect. Dis, 11 (7), 1160-1161. Brady, R., Wasson, A., Stirling, I., McAllister, C., & Damani, N. (2006). Is your phone bugged? The incidence of bacteria known to cause nosocomial infection on health care workers' mobile phones. The Journal of hospital infection, 62 (1), 123-125. Brown, R. B., Stechenberg, B., Sands, M., Hosmer, D., & Ryczak, M. (1987). Infections in a pediatric intensive care unit. Archives of Pediatrics and Adolescent Medicine, 141 (3), 267. Chin, K. R., Adams Jr, S. B., Khoury, L., & Zurakowski, D. (2005). Patient behavior if given their surgeon's cellular telephone number. Clinical orthopaedics and related research, 439, 260. Goldblatt J. G., M., Krief, I., Klonsky, T., Haller, D., Milloul, V., Sixsmith, D. M., . . . Potasman, I. (2007). Use of cellular telephones and transmission of pathogens by medical staff in New York and Israel. Infection control and hospital epidemiology, 28 (4), 500-503. Isaacs, D., Daley, A., Dalton, D., Hardiman, R., & Nallusamy, R. (1998). Swabbing computers in search of nosocomial bacteria. The Pediatric infectious disease journal, 17 (6), 533. Jayalakshmi, J., Appalaraju, B., & Usha, S. (2008). Cellphones as reservoirs of nosocomial pathogens. Journal of the Association of Physicians of India, 56, 388-389. Karabay, O., Koçoglu, E., & Tahtaci, M. (2007). The role of mobile phones in the spread of bacteria associated with nosocomial infections. J Infect Dev Ctries, 1, 72-73. Lapinsky, S. E., & Easty, A. C. (2006). Electromagnetic interference in critical care. Journal of critical care, 21 (3), 267-270. Milliken, J., Tait, G. A., Ford-Jones, E., Mindorff, C. M., Gold, R., & Mullins, G. (1988). Nosocomial infections in a pediatric intensive care unit. Critical care medicine, 16 (3), 233. MT, E., & IE, E. (2010). Mobile (Cellular) Phones Contamination with Nosocomial Pathogens in Intensive Care Units. Med. J. Cairo Univ, 78 (2), 1-5. Sepehri, G., Talebizadeh, N., Mirzazadeh, A., Mir-shekari, T. R., & Sepehri, E. (2009). Bacterial Contamination and Resistance to Commonly Used Antimicrobials of Healthcare Workers' Mobile Phones in Teaching Hospitals, Kerman, Iran. American Journal of Applied Sciences, 6 (5), 806-810. Srikanth, P., Rajaram, E., Sudharsanam, S., Lakshmanan, A., Mariappan, U. S. S., & Jagannathan, K. (2010). Mobile phones: emerging threat for infection control. Journal of Infection Prevention, 11 (3), 87-90. Tekerekoglu, M. S., Duman, Y., Serindag, A., Cuglan, S. S., Kaysadu, H., Tunc, E., & Yakupogullari, Y. (2011). Do mobile phones of patients, companions and visitors carry multidrug-resistant hospital pathogens? American journal of infection control, 39 (5), 383-385. Ulger, F., Esen, S., Dilek, A., Yanik, K., Gunaydin, M., & Leblebicioglu, H. (2009). Are we aware how contaminated our mobile phones with nosocomial pathogens? Annals of Clinical Microbiology and Antimicrobials, 8 (1), 7. Suggested Reading from Inquiries Journal
Inquiries Journal provides undergraduate and graduate students around the world a platform for the wide dissemination of academic work over a range of core disciplines. Representing the work of students from hundreds of institutions around the globe, Inquiries Journal's large database of academic articles is completely free. Learn more | Blog | Submit Latest in Health Science |